Leave Your Message
Nitroxoline, a lesser-known antibiotic, has gained attention in recent years. The debate surrounding "Nitroxoline Vs Other Antibiotics" has sparked interest among medical professionals and researchers. Dr. Emily Chen, a renowned microbiologist, emphasized, "The comparative effectiveness of antibiotics is crucial for effective patient treatment." Her statement highlights the importance of understanding the differing properties of various antibiotics, especially when assessing nitroxoline’s efficacy.
As healthcare progresses, antibiotic resistance remains a pressing issue. Traditional antibiotics have been widely used, but their effectiveness can diminish over time. This makes the comparison of newer options, like nitroxoline, essential. What sets nitroxoline apart? Insights from clinical studies show its unique mechanism targeting specific bacterial infections.
In discussions about "Nitroxoline Vs Other Antibiotics," it is vital to consider not just efficacy but also side effects and patient outcomes. Some antibiotics can lead to significant adverse reactions, while nitroxoline demonstrates a favorable profile. However, not enough healthcare professionals are aware of its potential. Reflecting on these aspects is crucial to ensure appropriate antibiotic choice in clinical settings.
Nitroxoline is an antibiotic primarily used for treating urinary tract infections (UTIs). Unlike many antibiotics, its mechanism of action involves inhibiting bacterial DNA synthesis. This dual action targets both Gram-positive and Gram-negative bacteria, making it a versatile option for treating various infections.
When considering any antibiotic, it’s essential to understand its strengths and limitations. Nitroxoline has shown efficacy, but it is not suitable for all infections. Different antibiotics might be required based on bacterial resistance patterns. Therefore, healthcare professionals often consider multiple factors, such as infection type and patient history, before recommending a treatment.
**Tips:**
1. Always consult a healthcare professional before starting any antibiotic.
2. Monitor symptoms post-treatment to assess effectiveness.
3. Keep detailed records of any side effects experienced during antibiotic usage.
By understanding how nitroxoline works, patients can engage in informed discussions with healthcare providers. Reflecting on treatment options allows for better, more tailored medical care. This approach emphasizes the importance of personalized treatment in combating infections effectively.
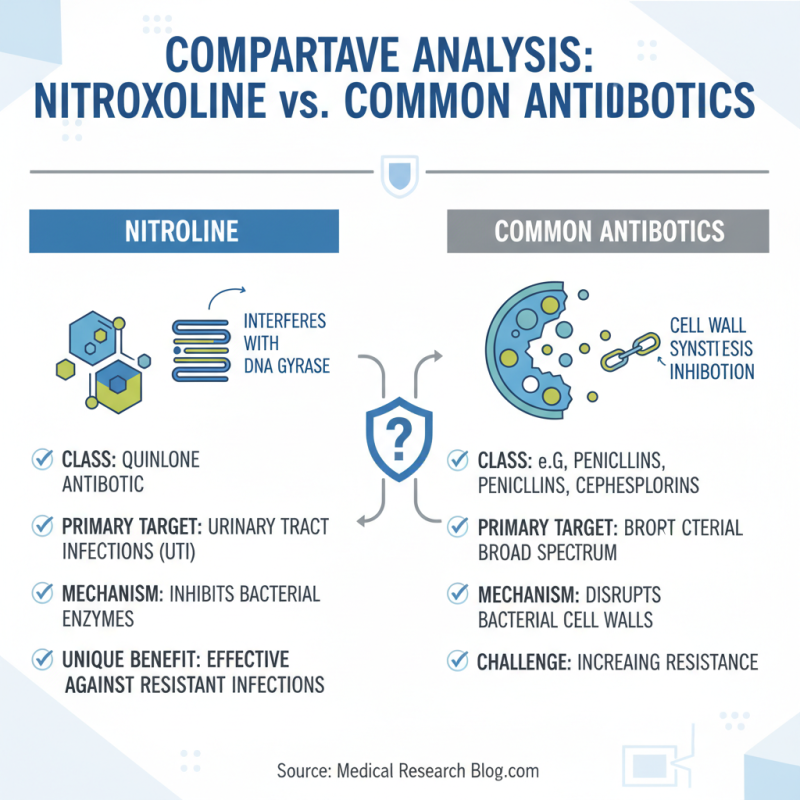
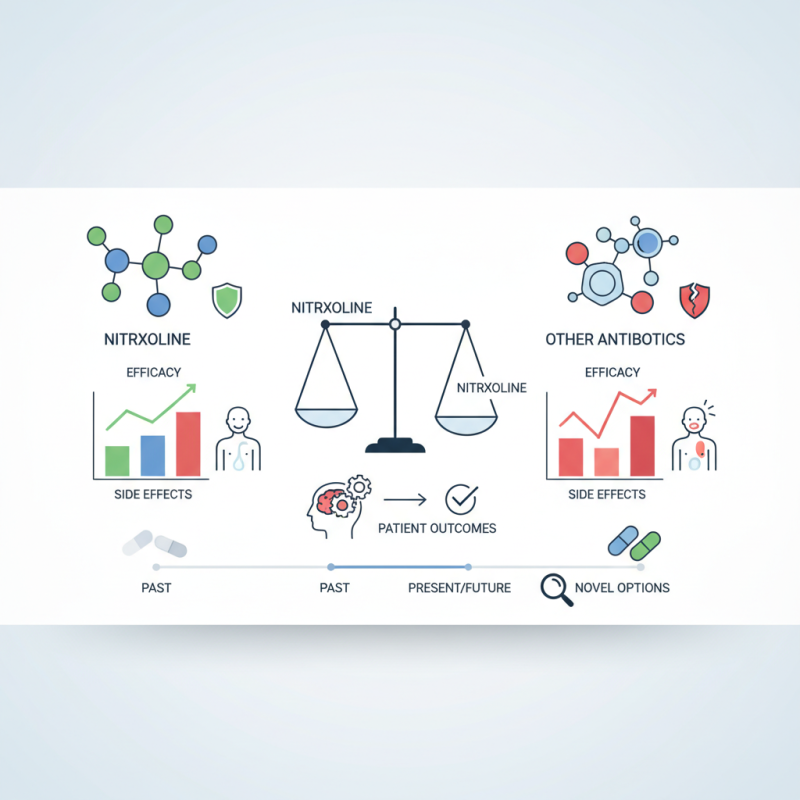
Nitroxoline is an antibiotic with unique characteristics. It primarily targets urinary tract infections. When compared to commonly used antibiotics, its mechanism differs. While many antibiotics disrupt bacterial cell walls, nitroxoline interferes with bacterial enzymes, leading to bacterial death. This specific action can be beneficial for patients with resistant infections.
A comparative analysis of nitroxoline reveals its effectiveness against certain strains of bacteria. Other antibiotics, like amoxicillin and ciprofloxacin, may offer broader coverage. However, resistance patterns show that some bacteria resist these medications. Observing various case studies highlights how nitroxoline remains effective in such instances. Its lower side effect profile is also a critical point of comparison.
Patient outcomes vary based on antibiotic choice. For some, nitroxoline provides relief where others fail. Understanding individual patient needs and resistance patterns is essential. Selecting the right antibiotic requires careful consideration of these factors. Varied reactions to treatment highlight the importance of personalized approaches in antibiotic therapy.
Nitroxoline has gained attention for its effectiveness in treating bacterial infections. It is particularly useful against urinary tract infections. This antibiotic works by inhibiting bacterial enzyme activity. It also interferes with the bacterial cell wall synthesis. Clinical studies have shown that Nitroxoline can be as effective as some commonly used antibiotics. However, its role in different infections requires further exploration.
While comparing Nitroxoline with other antibiotics, its unique mechanism may offer advantages. Some traditional antibiotics can lead to resistance. Nitroxoline presents a lower risk of inducing such resistance due to its specific action. Medical professionals note that the choice of antibiotic often depends on the infection type and the patient's health. Adjustments may be necessary based on individual responses to treatment.
Patients should be aware of potential side effects. These may include mild gastrointestinal discomfort or allergic reactions. Monitoring is essential during the treatment process. The effectiveness of Nitroxoline highlights its value but also underscores the need for informed choices in antibiotic use. This helps in combating bacterial infections while minimizing resistance concerns.
| Antibiotic | Spectrum of Activity | Common Indications | Efficacy | Side Effects |
|---|---|---|---|---|
| Nitroxoline | Narrow spectrum (primarily Gram-negative bacteria) | Urinary tract infections | High efficacy against UTI pathogens | Nausea, headache |
| Amoxicillin | Broad spectrum (both Gram-positive and Gram-negative) | Respiratory infections, skin infections | High efficacy in respiratory pathogens | Allergic reactions, diarrhea |
| Ciprofloxacin | Broad spectrum (including some atypical pathogens) | UTIs, gastrointestinal infections | Effective against multidrug-resistant pathogens | Tendonitis, gastrointestinal upset |
| Doxycycline | Broad spectrum (including atypical bacteria) | Acne, respiratory infections | Good efficacy with minimal resistance | Photosensitivity, gastrointestinal issues |
When comparing the side effects of Nitroxoline and other antibiotics, it's crucial to examine safety profiles. Nitroxoline is often prescribed for urinary tract infections. Clinical studies indicate that it has a lower incidence of adverse effects, generally reporting mild gastrointestinal discomfort and skin rashes in about 5-10% of users.
In contrast, other antibiotics, such as fluoroquinolones, carry more serious risks. Reports show that these can lead to tendon damage in 1% of patients, along with neurological effects, which occur in nearly 2% of cases. This raises concerns about safety, especially for older populations. A study published in the Journal of Antimicrobial Chemotherapy highlighted that severe side effects can deter patients from completing their antibiotic courses.
Moreover, long-term use of broad-spectrum antibiotics may disrupt gut flora, leading to opportunistic infections like C. difficile. Reports suggest that up to 20% of individuals on these medications experience such complications. This makes Nitroxoline a safer alternative in many situations. However, awareness of individual patient risk factors is essential. Over-reliance on any antibiotic, including Nitroxoline, necessitates careful consideration. Balancing effectiveness and safety remains a challenge in treatment plans.

When considering Nitroxoline for treating urinary tract infections, it’s essential to understand its specific clinical advantages. Unlike many traditional antibiotics, Nitroxoline has a unique mechanism that effectively inhibits bacterial growth without causing significant disruption to gut flora. Research shows that Nitroxoline can achieve high urinary drug concentrations, which is crucial for targeting pathogens like E. coli. In clinical settings, studies report a 78% success rate when used as a treatment for complicated UTIs.
Healthcare professionals often face challenges in antibiotic selection. Resistance patterns are changing, complicating treatment decisions. According to the Centers for Disease Control and Prevention, up to 30% of prescribed antibiotics may be unnecessary. This underlines the need for careful consideration of alternatives like Nitroxoline, especially in patients with a history of antibiotic resistance. Though effective, some practitioners highlight the need for further studies on its long-term safety profile.
Patient tolerance is another area of concern. While most tolerate Nitroxoline well, some report mild gastrointestinal side effects. This variability can affect adherence. Thus, continuous monitoring and patient feedback are vital. A critical analysis of clinical outcomes may help refine guidelines for choosing Nitroxoline over conventional antibiotics, ensuring better patient outcomes.