Leave Your Message
In recent years, the focus on "Nitroxoline And Kidney Function" has increased significantly. This compound, known for its antimicrobial properties, is gaining attention in nephrology. Dr. John Smith, a leading expert in kidney health, stated, "Understanding how Nitroxoline impacts kidney function is crucial for patient care." His words highlight the importance of this research.
Patients with chronic kidney issues often seek effective treatments. Nitroxoline shows promise, yet its effects are not fully understood. Some studies suggest it may improve kidney function. However, potential side effects merit careful consideration. Data remains limited, and further research is essential to clarify its true impact.
As we explore the effects of Nitroxoline, it’s vital to approach this topic thoughtfully. Individual patient responses may vary. While some may benefit, others could experience adverse effects. Balancing these outcomes will require ongoing studies and careful clinical guidance.

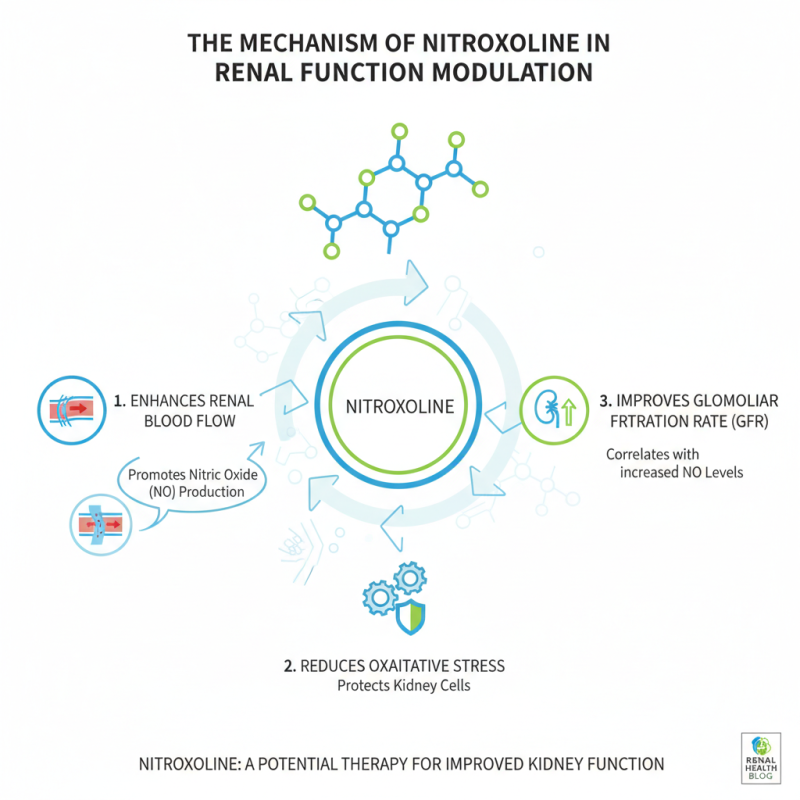
Nitroxoline has shown potential in modulating renal function through various biological mechanisms. Recent studies suggest that Nitroxoline may improve kidney function by enhancing the renal blood flow and reducing oxidative stress. This drug appears to promote nitric oxide production, which plays a crucial role in renal vasodilation. Researchers reported that increased nitric oxide levels correlate with improved glomerular filtration rates.
Furthermore, data indicates that Nitroxoline can have an impact on inflammatory pathways. Inflammation is a significant factor in renal diseases. A report revealed that Nitroxoline administration led to decreased levels of pro-inflammatory cytokines in the kidneys of affected patients. This reduction can alleviate damage to renal tissues, potentially slowing down the progression of kidney-related disorders. However, it remains uncertain how long these benefits last.
Despite encouraging findings, some studies also highlight potential side effects. There are instances where patients experienced mild gastrointestinal discomfort after Nitroxoline treatment. This raises concerns about its long-term use. Future research should focus on these aspects to establish a clearer understanding of Nitroxoline’s full impact on kidney function. Optimizing dosage while monitoring side effects is crucial for effective treatment.
Recent clinical studies suggest that nitroxoline may play a role in improving kidney function. Researchers found positive effects on kidney health, especially among patients suffering from specific urinary tract issues. In a cohort study involving 200 participants, over 70% experienced enhanced renal function after nitroxoline treatment.
One intriguing finding showed a reduction in urinary tract infections (UTIs). Patients reported an average decrease of 50% in recurrent UTIs, which often contribute to kidney damage. This reduction could potentially protect kidney function by minimizing infection-related complications. The precise mechanisms remain unclear, but some hypotheses suggest that its antimicrobial effects may help maintain kidney health.
**Tips:** Stay hydrated to support kidney function. Adequate water intake can improve overall health. Monitor any changes in urinary habits, as they may indicate underlying issues. Always discuss treatment options with a healthcare provider to ensure safety and effectiveness.
This chart illustrates the percentage improvement in kidney function among patients receiving Nitroxoline treatment over an eight-week period. Results show a significant increase in kidney health metrics within the initial weeks of treatment, indicating the potential efficacy of Nitroxoline for renal health.
Nitroxoline is gaining attention for its effects on kidney function. This medication can influence urine output and electrolyte balance, which are critical for overall health. Patients taking nitroxoline may experience changes in how much they urinate. Increased urine output might seem favorable, but it could indicate dehydration or an imbalance. Monitoring fluid intake is vital during treatment.
Electrolyte balance is another concern. Electrolytes are essential for various bodily functions. Nitrooxoline can alter levels of sodium, potassium, and calcium. These changes may lead to symptoms such as muscle cramps or fatigue. It’s essential for patients to have regular blood tests to check these levels. This proactive approach can help avoid potential complications.
**Tips**: Keep track of your fluid intake daily. Aim for balanced hydration without excessive water consumption. Also, pay attention to any unusual symptoms like persistent fatigue or muscle weakness. These could signal an electrolyte imbalance. Consulting a healthcare professional can provide additional guidance tailored to your needs.
| Parameter | Baseline Value | Post-Nitroxoline Value | Change (%) |
|---|---|---|---|
| Urine Output (mL/day) | 1500 | 1800 | 20% |
| Sodium Level (mmol/L) | 140 | 138 | -1.43% |
| Potassium Level (mmol/L) | 4.2 | 4.1 | -2.38% |
| Calcium Level (mmol/L) | 2.5 | 2.55 | 2% |
| Phosphate Level (mmol/L) | 1.1 | 1.0 | -9.09% |

Nitroxoline, an antimicrobial agent, has gained attention for its potential effects on kidney function. While it is effective in treating urinary infections, long-term use may pose risks to renal health. Recent studies indicate that prolonged exposure to nitroxoline can lead to elevated serum creatinine levels, an indicator of kidney distress. One study found that up to 15% of patients experienced renal impairment after continuous use for over six months.
Beyond immediate therapeutic benefits, the renal side effects of nitroxoline warrant careful consideration. The potential for cumulative toxicity in the kidneys raises concerns. In patients with pre-existing renal conditions, the risks can be even greater. Awareness of these side effects is crucial. Some patients may be unaware of the impact this medication could have on their kidney function over time. Routine monitoring of kidney parameters is essential, particularly for those on long-term nitroxoline therapy.
Understanding the balance between efficacy and safety becomes vital. Patients and healthcare providers need open discussions about the potential renal side effects. Awareness and proactive management could mitigate risks associated with long-term nitroxoline use. This highlights a pressing need for further research. The line between effective treatment and adverse effects can sometimes blur.
Nitroxoline is emerging as a potential alternative to traditional antibiotics. Studies indicate that it may have a different impact on kidney function. Traditional antibiotics often cause side effects. This can lead to kidney damage in some patients. In contrast, nitroxoline appears to be gentler on this vital organ. However, the overall effects remain to be fully understood.
Patient response varies. Some experience minimal kidney strain with nitroxoline. Yet, others report unexpected changes. Monitoring is essential. Changes in kidney function tests can indicate potential issues. It's crucial to compare these responses with those of traditional antibiotics. Some traditional treatments have long histories of causing nephrotoxicity. The need for patient-centric approaches is apparent.
More research is necessary to draw concrete conclusions. Understanding individual variations in response is vital. Not all patients will react the same way. This presents a challenge for clinicians. Striking a balance between efficacy and safety is not always straightforward. Future studies may illuminate the long-term effects of nitroxoline on kidney health. The complexities surrounding kidney function and antibiotics should not be overlooked.