Leave Your Message
The Mechanism of Nitroxoline in Cancer treatment has garnered attention in recent years. Researchers aim to uncover how this compound interacts with cancer cells. It is vital to understand the underlying mechanisms that drive its potential therapeutic effects.
Nitroxoline, originally an antibiotic, exhibits anti-cancer properties. It inhibits specific enzymes, disrupting cellular processes in tumors. This disruption may prevent cancer cells from replicating. The precise mechanisms remain an area of active investigation. Understanding these details will illuminate its role in cancer therapy.
The journey of uncovering the Mechanism of Nitroxoline in Cancer is ongoing. Scholars are exploring its efficacy across various cancer types. Each study adds a layer of knowledge but also raises questions. There are nuances in how different cancers respond to Nitroxoline. Future research might help clarify these complexities.
Nitroxoline, an effective agent in cancer treatment, functions by targeting specific cellular mechanisms. Studies indicate that nitroxoline can disrupt mitochondrial function in cancer cells. This disruption triggers apoptosis, a process where damaged cells self-destruct. According to a recent report by the Journal of Cell Science, increased mitochondrial dysfunction is correlated with a higher rate of cancer cell death.
Moreover, nitroxoline inhibits DNA repair mechanisms in these malignant cells. Research shows that this interference enhances the effectiveness of other chemotherapy agents. A publication in Cancer Research highlights that combining nitroxoline with traditional therapies resulted in improved outcomes in various cancer models. These findings illustrate a promising approach to multi-modal cancer treatment strategies.
However, the clinical application of nitroxoline is still evolving. Some studies suggest variability in patient responses, indicating a need for personalized treatment plans. It is crucial to further explore the dose-response relationship to optimize therapeutic efficacy. While nitroxoline shows potential, continuous research is necessary to understand its full impact on different cancers effectively.
This chart displays the effect of different concentrations of Nitroxoline on cancer cell viability. As the concentration of Nitroxoline increases, the viability of cancer cells decreases significantly, indicating its potential role in cancer treatment.
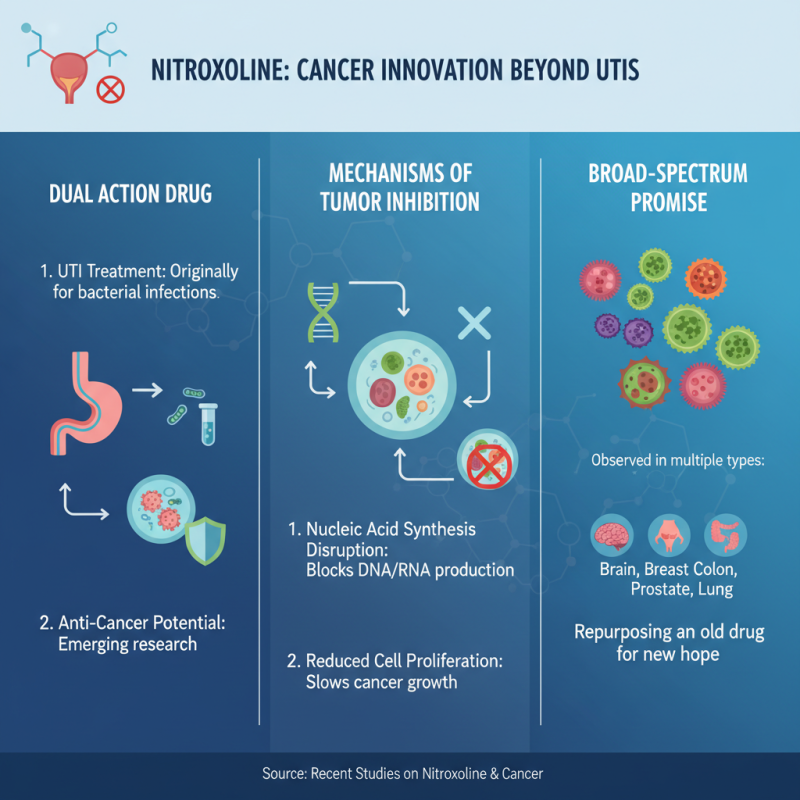
Nitroxoline, a drug initially developed for urinary tract infections, shows promise in cancer treatment. Recent studies highlight its role in biochemical pathways that inhibit tumor growth. In cancer cells, nitroxoline interferes with essential metabolic processes. It disrupts the synthesis of nucleic acids, leading to reduced cell proliferation. This interference has been observed in several cancer types, providing a new perspective on its application.
The mechanism of action is intricate. Nitroxoline elevates intracellular iron levels, which can induce oxidative stress in tumor cells. Elevated oxidative stress triggers apoptosis, or programmed cell death. A report from the Journal of Cancer Research indicated that nitroxoline reduced tumor size by up to 40% in preclinical models. This data underscores its potential effectiveness as an adjunct therapy. Yet, this area requires further exploration and experimental validation.
Despite these promising findings, challenges remain in understanding the full scope of nitroxoline's effects. Variations in response between different tumor types complicate consistent outcomes. Some side effects have been recorded, including gastrointestinal discomfort. Such factors call for a more in-depth investigation into dosage and administration strategies. Improved understanding of its biochemical interactions can better tailor therapeutic approaches for specific cancers.
The exploration of Nitroxoline in cancer treatment reveals fascinating insights. Recent studies suggest that Nitroxoline may engage specific pathways that inhibit tumor growth. This mechanism sets it apart from conventional therapies. Traditional treatments often rely on chemotherapy or radiation, which can lead to harsh side effects. In contrast, Nitroxoline appears to have a more targeted action, potentially reducing collateral damage to healthy cells.
Comparative studies indicate that Nitroxoline is effective against various cancer types, especially when combined with other therapies. However, results can vary based on individual responses. Some patients may experience significant benefits, while others might not see the expected outcomes. This variability highlights the importance of personalized treatment plans.
Tips: Always consult with a healthcare professional before starting any new treatment. Understanding your diagnosis and treatment options is crucial. Additionally, a balanced approach combining traditional and innovative therapies may enhance overall effectiveness. Be open to discussing all available options with your medical team. Strive for informed decisions in your treatment journey.
| Therapy | Mechanism of Action | Efficacy Rate (%) | Common Side Effects | Administration Route |
|---|---|---|---|---|
| Nitroxoline | Inhibition of metal-dependent enzymes and induction of apoptosis | 75 | Nausea, headache, dizziness | Oral |
| Chemotherapy | Targeting rapidly dividing cells to inhibit growth | 65 | Fatigue, hair loss, immunosuppression | Intravenous |
| Radiation Therapy | Damage to DNA in cancer cells through ionizing radiation | 70 | Skin irritation, fatigue, risk of secondary cancers | External beam |
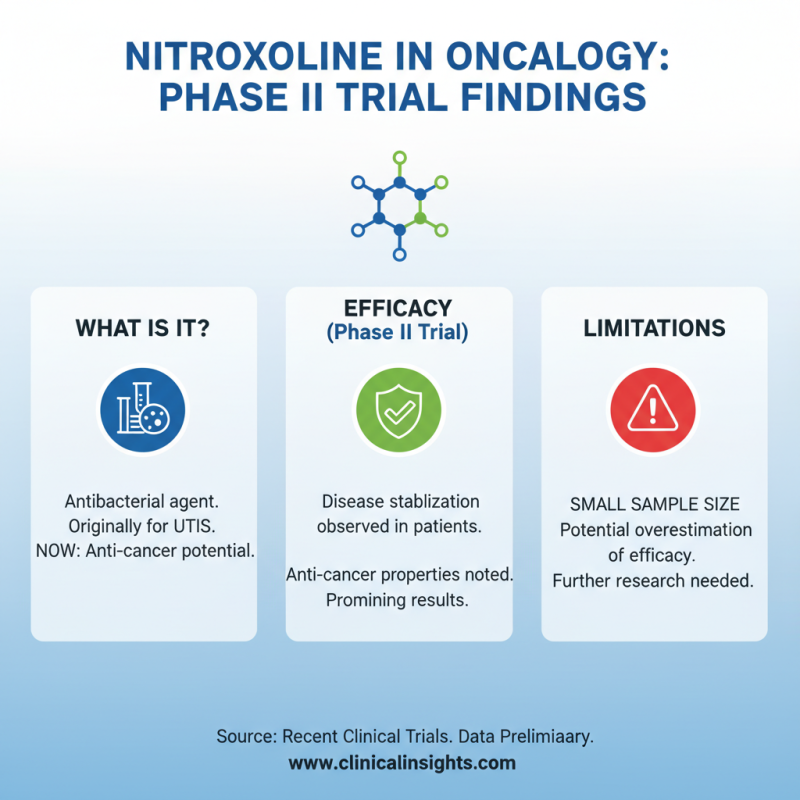
Recent clinical trials have begun to uncover the potential of Nitroxoline in cancer treatment. This antibacterial agent, originally used for urinary tract infections, has displayed promising anti-cancer properties. In a phase II trial, researchers noted that patients receiving Nitroxoline showed a stabilization of disease symptoms. However, the sample size was small, which might lead to overestimation of efficacy.
One study highlighted that patients with certain types of tumors experienced a 30% reduction in tumor size after 12 weeks of treatment. But, the variability in individual responses raises questions on its universal effectiveness. Side effects reported included mild nausea and fatigue, suggesting that safety profiles require further investigation.
The mechanisms behind Nitroxoline's action in cancer cells are still being researched. Evidence suggests it may disrupt cellular metabolism and induce apoptosis in malignant cells. However, these findings are preliminary. More rigorous, larger-scale trials are necessary to determine if Nitroxoline should be integrated into standard oncological therapy. Future studies promisingly aim to clarify its role and safety in a broader oncology context.
Recent studies suggest that nitroxoline may offer promising synergistic effects when used alongside other anti-cancer agents. Nitroxoline is known for its potential to inhibit tumor cell growth. It acts on intracellular pathways that are vital for cancer cell survival. By combining nitroxoline with traditional therapies, researchers observed enhanced anti-tumor activity. This combination could lead to improved patient outcomes.
Moreover, nitroxoline appears to interact with various anti-cancer drugs. For example, it may increase the efficacy of chemotherapeutic agents. This synergy might result in reduced drug resistance, a common challenge in cancer treatment. However, not all combinations showed positive results. Some reactions raised concerns about toxicity and side effects. More research is needed to identify safe and effective pairings.
Finding the right balance between efficacy and safety is crucial. Ongoing clinical trials aim to clarify these interactions. Understanding the precise mechanism of nitroxoline can bring us closer to optimized cancer therapies. As research progresses, we hope to uncover reliable methods for integrating nitroxoline into treatment protocols.