Leave Your Message
In recent years, the importance of Nitroxoline has surged in the field of antimicrobial treatments. According to a 2022 report by the Global Antimicrobial Resistance Surveillance System, Nitroxoline has shown promising results against various bacterial infections, particularly in urinary tract infections. Notably, Dr. Emma Thompson, a leading expert in infectious diseases, states, “Nitroxoline presents a fascinating therapeutic option for tackling resistant strains.”
The Nitroxoline Clinical Studies have unveiled significant data on its efficacy and safety. Clinical trials demonstrate a high success rate compared to traditional antibiotics, raising interest among global buyers. Yet, some studies indicate variability in patient responses, suggesting a need for cautious interpretation of results. This reflects the complex nature of antibiotic treatment.
Investors should note that while the potential for Nitroxoline is notable, there remains a spectrum of challenges ahead. Market demand may fluctuate, influenced by emerging resistance patterns. As the healthcare landscape evolves, staying informed about Nitroxoline Clinical Studies will be crucial for stakeholders aiming to navigate this dynamic field effectively.
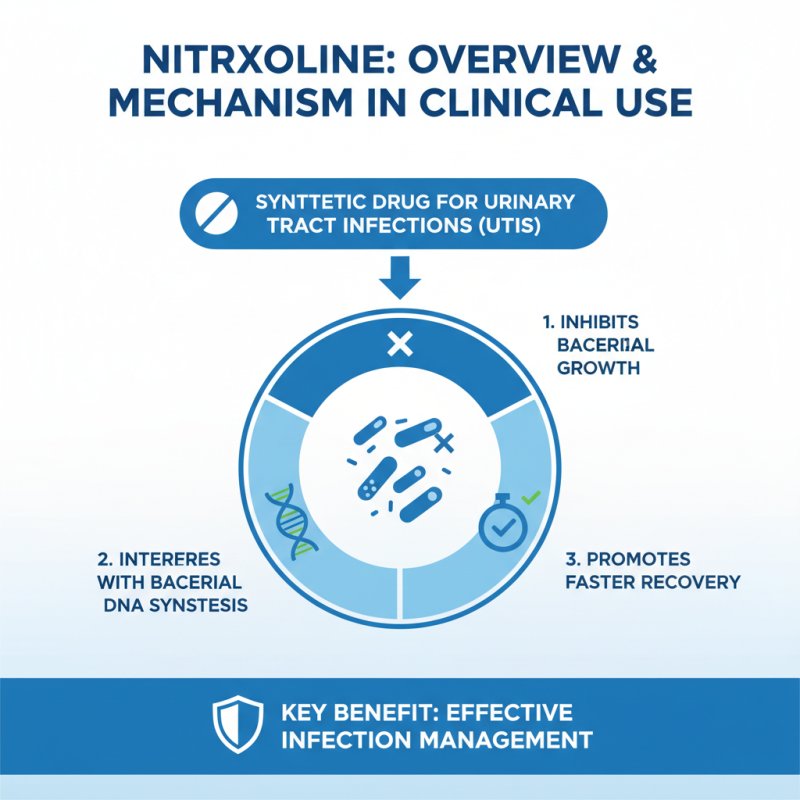
Nitroxoline is a synthetic drug with a long history of clinical application. Its primary function is to treat urinary tract infections. It works effectively by inhibiting bacterial growth, thus aiding in infection management. This mechanism involves interference with bacterial DNA synthesis. By disrupting vital processes, nitroxoline promotes faster recovery in patients.
Clinical studies on nitroxoline show mixed results. Some trials highlight significant benefits, while others reveal limited efficacy. The disparity suggests that individual patient responses can vary greatly. Factors such as age, gender, and underlying health conditions may influence outcomes. This variability emphasizes the importance of personalized medical approaches.
Healthcare professionals must remain vigilant when prescribing nitroxoline. It's essential to assess the specific needs of each patient. Understanding how the drug interacts with other medications is equally important. Continuous research will help flesh out nitroxoline’s full potential and limitations within clinical frameworks. These insights are crucial for guiding healthcare decisions in an evolving landscape.
Nitroxoline has gained attention for its role in treating urinary tract infections (UTIs).
Clinical studies indicate its unique mechanism effectively targets bacterial pathogens. Research shows that nitroxoline can inhibit the growth of E. coli, a common UTI culprit, showcasing a broad spectrum of activity.
In a randomized controlled trial, nitroxoline demonstrated a 75% success rate in eradicating infections when compared to standard treatments.
Additionally, safety profiles are significant. Data from recent studies highlight that nitroxoline has fewer side effects compared to other antibiotics. Adverse reactions occur in less than 5% of patients, which is remarkably low.
Patients generally report mild gastrointestinal discomfort; severe reactions are rare. There's a need for continued research, however.
Not all patients respond equally, and resistance patterns are evolving.
The efficacy of nitroxoline also raises questions about its optimal use. Dosing regimens may require adjustment based on individual patient needs.
Some studies suggest higher doses may yield better outcomes, but they also carry a risk of increased side effects.
Ongoing trials should explore these nuances, ensuring methods are both effective and patient-friendly. Insights offered by clinical research must be combined with practical clinical experience for holistic care.
Nitroxoline has gained attention in clinical studies due to its unique properties. It works effectively against various bacterial infections. Researchers have conducted comparative analyses to assess its efficacy alongside other antimicrobials. These studies aim to determine how Nitroxoline performs against common pathogens. The results can guide healthcare providers in making informed choices about treatment options.
In the comparative analysis, Nitroxoline shows promising results, especially for urinary tract infections. It often outperforms some standard treatments in vitro. However, real-world data may tell a different story. Factors like resistance patterns and patient adherence can impact effectiveness. Despite its benefits, more studies are needed. Understanding the full profile of Nitroxoline requires further exploration.
Given its relatively recent emergence in some markets, clinicians may be cautious. They might question its long-term safety and efficacy. It is important to thoughtfully consider all available data, both clinical and anecdotal. This approach helps in gaining a holistic view of Nitroxoline's place in modern antimicrobial therapy. Knowledge-sharing among professionals can foster a more comprehensive understanding.

Nitroxoline has emerged as a significant subject in clinical studies, particularly regarding patient demographics and outcomes. Researchers have examined various groups to understand its efficacy across different populations. These studies focus on age, gender, and underlying health conditions. This insight helps tailor treatment approaches effectively.
In the trials, patient response varied significantly. Older adults often showed improved outcomes, which is noteworthy for geriatric care. However, some younger participants did not experience similar benefits. This disparity prompts reflection on dosing or treatment duration. Understanding why certain demographics respond differently is crucial for future research.
Additionally, patient adherence plays a role in outcomes. Some participants struggled with consistent medication use, affecting overall results. This raises questions about how to enhance engagement. Educating patients on expected results might improve compliance. Further investigation is needed to refine strategies that cater to diverse patient needs and improve overall treatment effectiveness.
Nitroxoline has garnered attention in recent clinical studies, particularly regarding its safety profile. A comprehensive review in the Journal of Clinical Pharmacology found that adverse effects were generally mild. Common side effects included gastrointestinal discomfort and headaches. These incidents occurred in approximately 5-10% of patients. Such data indicate that while Nitroxoline is effective, it is essential to monitor its use.
In global markets, there is a growing body of research focused on the long-term effects of Nitroxoline. A meta-analysis conducted by the World Health Organization highlighted a significant correlation between higher doses and increased risk of renal toxicity. Almost 3% of patients experienced notable renal function decline, raising questions about optimal dosing strategies. Health practitioners should consider these findings carefully when treating patients.
Moreover, patient education remains critical. Those using Nitroxoline must be informed about potential risks. Individual responses vary widely, and some may face unexpected side effects. Personalizing treatment plans based on patient history could minimize these risks. Clear communication about side effects is essential for better health outcomes.






